 Dr. Chopra began by describing that pain in EDS generally comes from four sources: nerves (neuropathic), muscles (myofascial), joints (nociceptive), and headaches. He described how EDS causes each of these in turn. Muscles are held together by fascia, which is made of collagen. Muscles spasms and knots develop to compensate for the unbalanced and "wobbly" surrounding joints. Myofascial pain is a chronic form of muscle pain. When muscles are in spasm, they will develop knots (knots are actually minuscule tears in the muscle that release calcium and cause further contraction). They will also develop trigger points that cause additional spasms. These trigger points are painful and sensitive areas that can cause referred pain to other areas in the body. Trigger point injections work to release the muscle contractions--when a needle is places into the muscle, it will let go. Dry needling is one technique, however, Dr. Chopra recommends using a numbing medication. Manual techniques to stop contraction include myofascial release, muscle energy technique, strain-counter strain, and craniosacral therapy. Muscle relaxants can be used, but Dr. Chopra was not a huge fan of them (not as a long term solution, anyways), as they cause decreased tone and lethargy. Nerve pain (neuropathic pain) in those with EDS is attributed to the fact that nerves are made of connective tissue. This tissue is more fragile in EDSers, and the fragile nerves become over-stretched over time. Individuals with EDS also tend to suffer from small fiber neuropathy and complex regional pain syndrome (CRPS). In some cases, the nerve pain could be caused by a mitochondria disorder. The medications suggested by Dr. Chopra included gabapentin, pregablin, duloxetine, milnacipram, and antidepressants (tricyclic and SNRIs). SSRIs do not work for nerve pain. Headaches and neck pain become a problem in EDSers due to cerebrovascular reactivity--i.e. the blood vessels in the head are sensitive. Those with EDS are also prone to migraines and to increased intercranial pressure. Headaches may be from inside the head (migraines) or outside the head (chronic and tension). The treatment for each is different. There are many causes of neck pain in EDSers including C1-C2 instability, kyphosis of the neck, degeneration of neck disks, cranio-cervical instability, and chiari. For migraines, Dr. Chopra suggested that EDSers take abortive medications such as triptans. He also mentioned TMJ pain causing headaches. He recommended avoiding OTC night mouth guards (have custom ones made), and to tell yourself not to clench teeth at night before you fall asleep.
Dr. Chopra made some suggestions for the prevention of pain, including: - do not stand on one hip or sway hips
- do not stand on outside of feet
- do not sit in W formation
- do not hyperextend knees
- avoid repetitive activities
- keep work surfaces at an appropriate height
- use soft mattress
- use feather or memory foam pillow
- use grocery cart instead of bags
- keep handbags light
- keep clothing loose and light
- wear bras with wide straps and cross over straps
- wear light and soft shoes, use orthotics
Dr. Chopra mentioned low dose Naltrexone. This medication blocks the effects of opioids (opioid antagonist). It is beginning to be used for autoimmune disorders to help with pain. However, he has found that it helps with EDS patients as well. He gives doses normally starting at 2mg and increasing to 4.5mg per day. Dr. Chopra also recommended topicals, however, EDSers must make sure that ActiveMas or DMSO are added to the topical in order for it to penetrate the
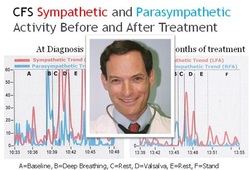 Dr. Pocinki began his talk giving a quick overview of the autonomic nervous system and autonomic dysfunction. After a poor nights sleep, many bodies respond by producing extra adrenaline to keep them going (as a side note, this is why clonidine works for ANS dysfunction--it suppresses adrenaline.) The ANS regulates all body processes that occur automatically including sleep. The ANS is classically divided into two subsystems: the parasympathetic nervous system (PNS--"rest and digest") and sympathetic nervous system (SNS--"fight or flight"). Dr. Pocinki began his theory of autonomic dysfunction in EDS. There is the concept of an adrenaline reserve. The reserve is the capacity of an individual to deal with stress, and it is not unlimited. The central paradox for those with hypermobile EDS and ANS dysfunction is that the lower the EDSers reserves are, the more exaggerated the stress response is. He used the metaphor of a car. A person with ANS dysfunction is constantly hitting the breaks and gas attempting to get his/her body where it need to be. Instead, this person is getting surges of too much gas/slam on breaks/too much gas/slam on breaks/too much gas....and on it goes. Thus, a person with ANS dysfunction wastes tons of energy regulating body processes that should be automatic. A sympathetic surge is marked by palpitations, shortness of breath, and a flushed face. Here, the gut relaxes. Conversely, in a parasypathetic surge, an individual will show signs of nausea and chills. Sustained SNS stress leads to pain, fatigue,and dehydration. This sustained stress also leads to depletion from the stressor-over-response cycle. The depletion phase is marked by trouble with concentration, a tendency to avoid tasks, trouble with details, and the like. Further depletion leads to sympathetic activity sufficient to mask pain. That is, the individual's resources are so depleted that an contradictory response happens--the individual will feel good, and have a lot of energy. He/she will also most likely have trouble sleeping at this phase. Finally, in the sustained parasympathetic response phase, i.e. the "tired but wired" phase, an individual will experience nausea, abdominal discomfort, malaise, fatigue, and lightheadedness. These symptoms will be constant.
Dr. Pocinki next posed the question: why do EDSers look like they have (and are diagnosed as having) psychological disorders? He reviewed the symptoms (under the DSM) of common psychological disorders, including panic attacks, panic disorder, ADHD, and hypomania (bipolar disorder). The descriptions of all of these in the DSM can describe much of the ANS dysfunction above as well.
Finally, Dr. Pocinki spoke about the treatment of ANS dysfunction, which means the treating physician must address the underlying problems. Sleep is a patient's only chance to, metaphorically, put gas in his or her tank. If the patient does not get his or her pain under control, the patient will never get decent sleep. The energy used during the day (that must be replaced by sleep) consists of pain, fatigue, dehydration, cognitive effort, emotional stress, and other (work, school, etc.)
Though this talk had a focus on the Vascular Type of EDS (VEDS), Dr. Black covered vascular issues that could effect all EDSers. The types of vascular issues that are most common in EDS, especially VEDS, are aneurysm, dissection, and pseudoaneuysm. However, those with EDS can suffer from a spectrum of arterial and venous anomalies including spontaneous dissection and rupture. These issues are VASTLY under-reported in non-vascular EDS cases. According to him, much more research most be done on vascular issues in the other types of EDS. In most cases of patients with VEDS or EDS with vascular issues, an echo-cardiogram is recommended at the age of ten, and then every 5 years thereafter. If an abnormality is found on the echo, Dr. Black recommends follow-up scans every 6 months.
Dr. Black spoke a bit about a new-ish medication, celiprolol (not currently available in the US). The effect of celiprolol on prevention of cardiovasular events in VEDS has been favorable, as it seems to dilate the blood vessels of VEDS patients. However, it is only available in Canada and the EU so far.
Dr. Black does recommend a low-dose beta blocker to all patients with vascular issues. However, there are exercise implications for many patients. He suggests that patients on a beta blocker use a polar heart rate monitor if they are engaging in strenuous exercise. If the patient's baseline heart rate increases by more than 50%, the patient must stop exercise.
 Dr. Qutab began his talk by explaining a bit about NF-kappaB. NF-kB is a protein complex that controls the transcription of DNA. It is found in almost all animal cell types and is involved in cellular responses to stimuli such as stress, cytokines, free radicals, ultraviolet irradiation, oxidized LDL, and bacterial or viral antigens. NF-kB is in the cytosol where it is made inactive by Inhibitory kappaB. However, exposure to stressful stimuli activates inhibitory kappaB kinase, which destroys the IkB. Once destroyed, the NF-KB is able to bind with DNA. The genes within the DNA then encode for increased production of inflammatory materials. Thus far, diseases such a MS, Lupus, IBS, and the like have been associated with the activation of NF-KB.The triggers for the activation of NF-kB are stress, radiation, injury, leaky gut, food and environmental allergies, vitamin D deficiency, among others. A person's total toxic exposure is comprised of physical sources (injury), nutritional sources, chemical sources (xenobiotics, organics), and infection (endo- and exotoxins). Exotoxins are such things as pesticides, synthetic materials, synthetic medicines, additives, etc. Thus, the goal is to modulate inflammatory mediators in order to halt the pro-inflammatory genes that activate enzymes and cytokines to create inflammation and disease. Dr. Qutab also spoke briefly on NSAIDS and why he does not suggest them for EDSers. NSAIDS block the pathways to build cartilage. He is also strongly in favor of Vioxx staying off of the market. He believes that the treatment for pain and inflammation should be as follows: --remove ongoing triggers --optimize GI health --identify potential antecedents --modify mediators --introduce an anti-inflammatory diet --optimize fatty acids and eicosanoid synthesis --get enough vitamin D --phytonutritional modulation of NF-KB --restore structural integrity and remove subluxation --chrondo support --botantical angelgesics: white willow bark, boswellia, Devil's claw, etc. --proteolytic enzymes for acute/chronic pain and inflamation (curcumin, etc.)
His PowerPoint can be found here
Hello fellow EDSers and those looking for EDS resources! I promise I will get back to putting my conference notes up here very, very soon. I had a death in my family this week, and all of my energy has been spent doing things other than transcribing notes, unfortunately. However, I wanted to let you know that I did not forget about you or this site. New notes will be coming soon!
Dr. Rodney Grahame led the first plenary session on Friday morning. He first noted that in 2010, the hypermobile type and joint hypermobility syndrome (JHS) are finally being recognized as the same syndrome. A number of journal articles have made it clear that these two syndromes are very difficult to tell apart. He also mentioned that he is dismayed at the misdiagnoses by rheumatologists for EDS. Dr. Grahame stated that there is an atypical nature of pain in EDS, which causes the misdiagnoses. The G.I. involvement, as well is the atypical nature of pain, lead to symptoms of not being believed, or being ascribed to a psychological cause. He emphasized that to be told a genuine symptom of a recognized disease is unreal if the "most unkind cut of all." However, Dr. Grahame did note that there is a movement with in the specialty of rheumatology to recognize EDS, in part based on his tireless work and the work of many of the other speakers here.
Dr. Grahame then began to speak on this topic of "what should we call our syndrome?". He first spoke briefly about the problem with an eponymous disease. For EDS, the funny thing is that the men it was named after, Ehlers and Danlos, were not the first people to recognize the disorder. The first report of EDS was actually from Russia by An Chernogubov. Francis Parkes-Weber suggested the name of Ehlers-Danlos syndrome in 1938 (without doing his homework, apparently).
Dr. Grahame talked a bit about hypermobile EDS versus joint hypermobility syndrome. Dr. Grahame emhasized that JHS is only one aspect of the disorder. However, they have been seen as two different disorders for many years. Finally, in a 2009 article, Bradley Tinkle, et al., came to the conclusion that EDS hypermobile type and HMS are indistinguishable. The authors of this article were from three different continents. It was of their collective opinion that they would be helping patients by uniting the two different disorders.
Dr. Grahame did note the problems of the union of HMS into EDS. If a patient is diagnosed with EDS, the diagnosing physician may be accused of over-medicalizing symptoms and causing unnecessary anxiety. However if the patient is diagnosed with a HMS/JHS, the diagnosing physician is telling the patient that the problem is in their joints only, which is not true. The diagnosis of HMS/JHS also trivializes the syndrome and can have a detrimental effect on disability applications.
So getting back to the main question, a new name should be succinct, meaningful, and reveal the core characteristics of the syndrome. First, a keyword is ELASTICITY. Another keyword is DNA. Finally, this is a multi-systemic SYNDROME. So, for short, how about EDS?
Elliot Clark, the then-chairman and now chair emeritus, made the opening statements to the conference. I wanted to make this it's own post because there were a few quotes that I wrote down that I really loved:
--"EDS is far more normal than normal people think."
--"If you have kids, or plan to, get them evaluated for EDS as early as possible to manage symptoms."
"I've heard many others say, 'these are the few days [of the conference] where I get to feel NORMAL [being among others with EDS].'"
Dr. Clair Francomano led a main session entitled "What is new in EDS 2013." She reviewed the recent publications, which I will list here (a better list will be in her PowerPoint presentation--I was only able to write the gist of the titles before the slide was changed.)
--Dordoni: Recurring and generalized visceroptosis in EDSIII. A study of prolapse in hypermobility cases.
--Mayo Clinic: POTS--a heterogeneous and multifactorial disorder
--Castori: Mgmt of pain and fatigue in EDSIII. A study of the causes of pain and fatigue.
--Propriception article: Do people with BJHS and EDS have reduced proprioception. Found that they do have decreased position sense in the lower extremities, however, the evidence was not as good for upper extremities.
--De Paepe: EDS-a disorder with many faces. Review of genes and phenotypes. Examples of clinical cases
--Italian group (Castori, Dordoni): Study of gait. 3D gait analysis of individuals with EDS (pelvis, ankle, distal joints).
--Castori: Ehlers-Danlos Syndrome, Hypermobility Type: An Underdiagnosed Hereditary Connective Tissue Disorder with Mucocutaneous, Articular, and Systemic Manifestations
--Dermal ultrastructure in low Beighton Score members of 17 families with EDSIII. Changes in collagen were found in the low Beighton score family members. Called "non-hypermobile, hypermobile EDS."
De Paepe: Classic EDS type research regarding genes. Discussion of how old type I should be "Classic" and old Type II and Type III together should be considered "Hypermobile."
Dr. Francomano also mentioned that the cost of DNA sequencing has been cut from $1 billion to $10,000 per genome. NIH had 3 sequencing centers (Mendel project). There is also a family foundation funding 50 exomes with DNA samples. She spoke here about Dr. Schvink in Los Angeles and CSF leaks. CSF leaks can manifest as a headache with a rapid leak of fluid from the ear or nose.
Moving on to topics that she find interesting/concerning, Dr. Francomano began the next section of her speech by talking about neurological symptoms of EDS. She spoke briefly about the cranial cervical junction and compression of nerves (as this was covered in depth by Dr. Henderson). The cranial cervical junction can cause a number of problems in EDS patients, as it tends to become unstable over time.
She also mentions that many individuals with EDS have increased intercranial pressure, but she and other physicians are not certain why this is. This condition causes increased pressure on the lumbar puncture, and is potentially caused by a number of secondary conditions, including chiari. It is responsive to diamox therapy; however, bicarbonate levels must be monitored.
Further, she spoke on mast cell disease. A subset of patients have EDS, but also have flushing, hives, and anaphylaxis. However, many of these patients respond to therapy for mast cell activation disorder (including H1 and H2 blockers).
She mentioned that EDSers do not metabolize drugs as expected. Those with EDS are slow to respond to -caine derivatives (lidocaine, etc.); although there are a few who will over-respond to these medications and the effects will last for much longer than expected. Make sure to tell your dentist that you have EDS and, if possible, take a handout from the EDNF site. Additionally, the metabolism of other drugs in EDS patients tends to be accelerated or prolonged.
Finally, she spoke on inflammation. Inflammation has been found to be a component of osteoarthritis, even though most think of osteoarthritis as "bone on bone." It is also a part of mast cell disease, and it increases with higher insulin levels.
|





 RSS Feed
RSS Feed